Does Scar Tissue Register As Body Fat When Measured
| Adipose tissue | |
|---|---|
 Adipose tissue is 1 of the main types of connective tissue. | |
 Morphology of three different classes of adipocytes. | |
| Pronunciation | ( |
| Identifiers | |
| MeSH | D000273 |
| FMA | 20110 |
| Anatomical terminology [edit on Wikidata] | |
Adipose tissue, body fat, or simply fat is a loose connective tissue composed mostly of adipocytes.[ane] In add-on to adipocytes, adipose tissue contains the stromal vascular fraction (SVF) of cells including preadipocytes, fibroblasts, vascular endothelial cells and a variety of immune cells such as adipose tissue macrophages. Adipose tissue is derived from preadipocytes. Its chief role is to shop energy in the form of lipids, although it too cushions and insulates the body. Far from being hormonally inert, adipose tissue has, in contempo years, been recognized as a major endocrine organ,[two] equally information technology produces hormones such as leptin, estrogen, resistin, and cytokines (especially TNFα). In obesity, adipose tissue is also implicated in the chronic release of pro-inflammatory markers known as adipokines, which are responsible for the evolution of metabolic syndrome, a constellation of diseases including, but not express to, blazon two diabetes, cardiovascular affliction and atherosclerosis.[3] The two types of adipose tissue are white adipose tissue (WAT), which stores free energy, and brown adipose tissue (BAT), which generates torso heat. The formation of adipose tissue appears to be controlled in part by the adipose factor. Adipose tissue – more than specifically brown adipose tissue – was get-go identified by the Swiss naturalist Conrad Gessner in 1551.[4]
Anatomical features [edit]

Distribution of white adipose in the human body
In humans, adipose tissue is located: beneath the pare (subcutaneous fatty), around internal organs (visceral fat), in os marrow (yellow bone marrow), intermuscular (Muscular system) and in the chest (breast tissue). Adipose tissue is found in specific locations, which are referred to as adipose depots. Autonomously from adipocytes, which contain the highest percent of cells within adipose tissue, other cell types are nowadays, collectively termed stromal vascular fraction (SVF) of cells. SVF includes preadipocytes, fibroblasts, adipose tissue macrophages, and endothelial cells.
Adipose tissue contains many pocket-sized blood vessels. In the integumentary arrangement, which includes the pare, it accumulates in the deepest level, the subcutaneous layer, providing insulation from heat and common cold. Around organs, it provides protective padding. However, its main part is to be a reserve of lipids, which tin can be oxidised to meet the energy needs of the torso and to protect it from excess glucose past storing triglycerides produced by the liver from sugars, although some bear witness suggests that most lipid synthesis from carbohydrates occurs in the adipose tissue itself.[5] Adipose depots in different parts of the trunk accept different biochemical profiles. Under normal weather, it provides feedback for hunger and nutrition to the brain.
Mice [edit]
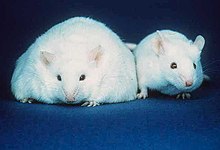
The obese mouse on the left has big stores of adipose tissue. Information technology is unable to produce the hormone leptin. This causes the mouse to be hungry and consume more than, which results in obesity. For comparison, a mouse with a normal amount of adipose tissue is shown on the right.
Mice have 8 major adipose depots, four of which are within the abdominal crenel.[1] The paired gonadal depots are attached to the uterus and ovaries in females and the epididymis and testes in males; the paired retroperitoneal depots are found along the dorsal wall of the abdomen, surrounding the kidney, and, when massive, extend into the pelvis. The mesenteric depot forms a glue-like web that supports the intestines and the omental depot (which originates near the tum and spleen) and - when massive - extends into the ventral abdomen. Both the mesenteric and omental depots incorporate much lymphoid tissue every bit lymph nodes and milky spots, respectively.
The two superficial depots are the paired inguinal depots, which are institute anterior to the upper segment of the hind limbs (underneath the pare) and the subscapular depots, paired medial mixtures of brown adipose tissue adjacent to regions of white adipose tissue, which are found under the pare between the dorsal crests of the scapulae. The layer of brown adipose tissue in this depot is often covered by a "frosting" of white adipose tissue; sometimes these two types of fat (dark-brown and white) are hard to distinguish. The inguinal depots enclose the inguinal group of lymph nodes. Minor depots include the pericardial, which surrounds the center, and the paired popliteal depots, between the major muscles behind the knees, each containing one large lymph node.[half-dozen] Of all the depots in the mouse, the gonadal depots are the largest and the virtually easily dissected,[7] comprising well-nigh thirty% of dissectible fat.[8]
Obesity [edit]
In an obese person, excess adipose tissue hanging downwards from the abdomen is referred to as a panniculus. A panniculus complicates surgery of the morbidly obese individual. It may remain as a literal "apron of skin" if a severely obese person loses large amounts of fat (a mutual effect of gastric featherbed surgery). Obesity is treated through practice, diet, and behavioral therapy. Reconstructive surgery is ane aspect of treatment.[9]
Visceral fat [edit]
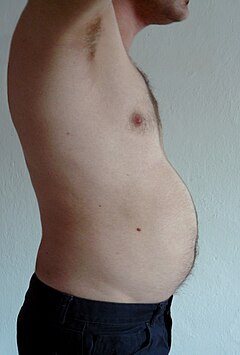
Visceral fatty or intestinal fat[10] (too known as organ fat or intra-abdominal fat) is located inside the abdominal cavity, packed between the organs (stomach, liver, intestines, kidneys, etc.). Visceral fatty is different from subcutaneous fat underneath the skin, and intramuscular fatty interspersed in skeletal muscles. Fat in the lower body, equally in thighs and buttocks, is subcutaneous and is not consistently spaced tissue, whereas fat in the abdomen is more often than not visceral and semi-fluid.[11] Visceral fat is equanimous of several adipose depots, including mesenteric, epididymal white adipose tissue (EWAT), and perirenal depots. Visceral fatty is oft expressed in terms of its area in cm2 (VFA, visceral fatty area).[12]
An excess of visceral fatty is known as central obesity, or "abdomen fatty", in which the abdomen protrudes excessively. New developments such every bit the Body Volume Index (BVI) are specifically designed to measure abdominal volume and abdominal fat. Excess visceral fat is too linked to type 2 diabetes,[thirteen] insulin resistance,[xiv] inflammatory diseases,[15] and other obesity-related diseases.[16] Also, the aggregating of cervix fat (or cervical adipose tissue) has been shown to exist associated with mortality.[17] Several studies have suggested that visceral fat tin be predicted from simple anthropometric measures,[eighteen] and predicts mortality more accurately than body mass alphabetize or waist circumference.[19]
Men are more likely to have fat stored in the abdomen due to sex activity hormone differences. Female sex hormone causes fatty to be stored in the buttocks, thighs, and hips in women.[20] [21] When women reach menopause and the estrogen produced by the ovaries declines, fat migrates from the buttocks, hips and thighs to the waist;[22] later fat is stored in the abdomen.[11]
Visceral fat tin be caused past excess cortisol levels.[23] At least 10 MET-hours per week of aerobic do leads to visceral fatty reduction in those without metabolic-related disorders.[24] Resistance grooming and caloric brake also reduce visceral fatty, although their effect may not be cumulative.[25] Both practise and hypocaloric nutrition cause loss of visceral fat, merely exercise has a larger consequence on visceral fat versus total fatty.[26] High-intensity exercise is one style to effectively reduce total abdominal fat.[27] [28] An free energy restricted diet combined with exercise will reduce full body fatty and the ratio of visceral adipose tissue to subcutaneous adipose tissue, suggesting a preferential mobilization for visceral fatty over subcutaneous fat.[29]
Epicardial fat [edit]
Epicardial adipose tissue (Consume) is a particular course of visceral fat deposited effectually the middle and establish to exist a metabolically agile organ that generates diverse bioactive molecules, which might significantly affect cardiac office.[30] Marked component differences take been observed in comparison EAT with subcutaneous fat, suggesting a location-specific touch of stored fat acids on adipocyte role and metabolism.[31]
Subcutaneous fat [edit]
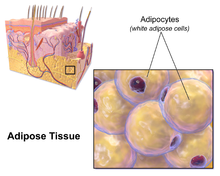
Micro-anatomy of subcutaneous fat
Most of the remaining nonvisceral fatty is institute just below the peel in a region called the hypodermis.[32] This subcutaneous fat is not related to many of the classic obesity-related pathologies, such as heart illness, cancer, and stroke, and some evidence even suggests it might exist protective.[33] The typically female (or gynecoid) blueprint of trunk fat distribution effectually the hips, thighs, and buttocks is subcutaneous fatty, and therefore poses less of a wellness risk compared to visceral fat.[34] [35]
Like all other fatty organs, subcutaneous fatty is an agile part of the endocrine system, secreting the hormones leptin and resistin.[32]
The relationship between the subcutaneous adipose layer and total torso fat in a person is often modelled by using regression equations. The well-nigh popular of these equations was formed by Durnin and Wormersley, who rigorously tested many types of skinfold, and, every bit a event, created ii formulae to calculate the body density of both men and women. These equations present an changed correlation between skinfolds and body density—as the sum of skinfolds increases, the body density decreases.[36]
Factors such as sexual activity, age, population size or other variables may make the equations invalid and unusable, and, every bit of 2012[update], Durnin and Wormersley'south equations remain only estimates of a person's true level of fatness. New formulae are nevertheless being created.[36]
Marrow fat [edit]
Marrow fat, besides known as marrow adipose tissue (MAT), is a poorly understood adipose depot that resides in the bone and is interspersed with hematopoietic cells as well equally bony elements. The adipocytes in this depot are derived from mesenchymal stem cells (MSC) which tin can give rise to fat cells, bone cells too as other prison cell types. The fact that MAT increases in the setting of calorie restriction/ anorexia is a feature that distinguishes this depot from other fat depots.[37] [38] [39] Exercise regulates MAT, decreasing MAT quantity and diminishing the size of marrow adipocytes.[forty] [41] [42] The practice regulation of marrow fat suggests that it bears some physiologic similarity to other white adipose depots. Moreover, increased MAT in obesity further suggests a similarity to white fat depots.[twoscore]
Ectopic fatty [edit]
Ectopic fat is the storage of triglycerides in tissues other than adipose tissue, that are supposed to incorporate simply small amounts of fatty, such as the liver, skeletal musculus, heart, and pancreas.[1] This can interfere with cellular functions and hence organ function and is associated with insulin resistance in type-ii diabetes.[43] It is stored in relatively high amounts effectually the organs of the abdominal cavity, but is not to be dislocated with visceral fat.
The specific crusade for the accumulation of ectopic fatty is unknown. The crusade is probable a combination of genetic, environmental, and behavioral factors that are involved in excess energy intake and decreased physical activeness. Substantial weight loss can reduce ectopic fat stores in all organs and this is associated with an improvement of the function of those organs.[43]
In the latter case, non-invasive weight loss interventions similar diet or exercise can decrease ectopic fat (especially in heart and liver) in overweight or obese children and adults.[44] [45]
Physiology [edit]
Complimentary fatty acids (FFAs) are liberated from lipoproteins past lipoprotein lipase (LPL) and enter the adipocyte, where they are reassembled into triglycerides by esterifying them onto glycerol. Human fatty tissue contains almost 87% lipids.[46]
There is a constant flux of FFAs inbound and leaving adipose tissue. The net direction of this flux is controlled by insulin and leptin—if insulin is elevated, then there is a net inward flux of FFA, and only when insulin is low can FFA leave adipose tissue. Insulin secretion is stimulated by high blood saccharide, which results from consuming carbohydrates.[47]
In humans, lipolysis (hydrolysis of triglycerides into gratuitous fatty acids) is controlled through the balanced command of lipolytic B-adrenergic receptors and a2A-adrenergic receptor-mediated antilipolysis.
Fat cells accept an important physiological office in maintaining triglyceride and free fat acid levels, as well as determining insulin resistance. Intestinal fat has a different metabolic profile—being more prone to induce insulin resistance. This explains to a large degree why central obesity is a marker of impaired glucose tolerance and is an independent risk gene for cardiovascular affliction (fifty-fifty in the absence of diabetes mellitus and hypertension).[48] Studies of female monkeys at Wake Forest University (2009) discovered that individuals suffering from higher stress have higher levels of visceral fat in their bodies. This suggests a possible cause-and-issue link between the 2, wherein stress promotes the aggregating of visceral fatty, which in plow causes hormonal and metabolic changes that contribute to heart disease and other health problems.[49]
Recent advances in biotechnology have allowed for the harvesting of adult stalk cells from adipose tissue, allowing stimulation of tissue regrowth using a patient's ain cells. In add-on, adipose-derived stem cells from both human being and animals reportedly can be efficiently reprogrammed into induced pluripotent stem cells without the demand for feeder cells.[l] The use of a patient's own cells reduces the chance of tissue rejection and avoids ethical issues associated with the use of man embryonic stalk cells.[51] A growing body of evidence too suggests that different fatty depots (i.e. abdominal, omental, pericardial) yield adipose-derived stem cells with different characteristics.[51] [52] These depot-dependent features include proliferation rate, immunophenotype, differentiation potential, gene expression, every bit well as sensitivity to hypoxic culture conditions.[53] Oxygen levels seem to play an important office on the metabolism and in full general the function of adipose-derived stem cells.[54]
Adipose tissue is a major peripheral source of aromatase in both males and females, contributing to the product of estradiol.[55]
Adipose derived hormones include:
- Adiponectin
- Resistin
- Plasminogen activator inhibitor-1 (PAI-1)
- TNFα
- IL-6
- Leptin
- Estradiol (E2)
Adipose tissues as well secrete a type of cytokines (jail cell-to-prison cell signalling proteins) called adipokines (adipose cytokines), which play a office in obesity-associated complications. Perivascular adipose tissue releases adipokines such as adiponectin that touch on the contractile function of the vessels that they surroundings.[1] [56]
Brownish fat [edit]

Chocolate-brown fat or brown adipose tissue (BAT) is a specialized form of adipose tissue important for adaptive thermogenesis in humans and other mammals. BAT can generate heat by "uncoupling" the respiratory chain of oxidative phosphorylation inside mitochondria through tissue-specific expression of uncoupling protein 1 (UCP1).[57] BAT is primarily located effectually the neck and large blood vessels of the thorax, where it may effectively act in heat exchange. BAT is robustly activated upon common cold exposure by the release of catecholamines from sympathetic fretfulness that results in UCP1 activation. BAT activation may also occur in response to overfeeding.[58] UCP1 activity is stimulated by long chain fatty acids that are produced subsequent to β-adrenergic receptor activation.[57] UCP1 is proposed to function as a fatty acid proton symporter, although the exact mechanism has notwithstanding to be elucidated.[59] In contrast, UCP1 is inhibited by ATP, ADP, and GTP.[sixty]
Attempts to simulate this process pharmacologically have so far been unsuccessful. Techniques to manipulate the differentiation of "brown fat" could get a mechanism for weight loss therapy in the future, encouraging the growth of tissue with this specialized metabolism without inducing it in other organs. A review on the eventual therapeutic targeting of dark-brown fat to treat man obesity was published by Samuelson and Vidal-Puig in 2020.[61]
Until recently, brown adipose tissue in humans was idea to be primarily limited to infants, but new evidence has overturned that belief. Metabolically active tissue with temperature responses similar to chocolate-brown adipose was beginning reported in the neck and trunk of some man adults in 2007,[62] and the presence of brown adipose in human adults was after verified histologically in the aforementioned anatomical regions.[63] [64] [65]
Beige fat and WAT browning [edit]
Browning of WAT, also referred to as "beiging", occurs when adipocytes within WAT depots develop features of BAT. Beige adipocytes take on a multilocular appearance (containing several lipid droplets) and increment expression of uncoupling poly peptide ane (UCP1).[66] In doing and so, these normally energy-storing adipocytes become energy-releasing adipocytes.
The calorie-burning capacity of brownish and biscuit fat has been extensively studied as inquiry efforts focus on therapies targeted to treat obesity and diabetes. The drug 2,4-dinitrophenol, which also acts every bit a chemic uncoupler similarly to UCP1, was used for weight loss in the 1930s. Yet, it was quickly discontinued when excessive dosing led to adverse side effects including hyperthermia and death.[66] β3 agonists, like CL316,243, accept also been developed and tested in humans. However, the apply of such drugs has proven largely unsuccessful due to several challenges, including varying species receptor specificity and poor oral bioavailability.[67]
Common cold is a primary regulator of BAT processes and induces WAT browning. Browning in response to chronic cold exposure has been well documented and is a reversible process. A report in mice demonstrated that cold-induced browning can be completely reversed in 21 days, with measurable decreases in UCP1 seen within a 24-hour period.[68] A study by Rosenwald et al. revealed that when the animals are re-exposed to a cold environs, the aforementioned adipocytes will adopt a beige phenotype, suggesting that beige adipocytes are retained.[69]
Transcriptional regulators, besides as a growing number of other factors, regulate the consecration of beige fat. Four regulators of transcription are central to WAT browning and serve equally targets for many of the molecules known to influence this process.[70] These include peroxisome proliferator-activated receptor gamma (PPARγ), PRDM16,[71] peroxisome proliferator-activated receptor gamma coactivator 1 alpha (PGC-1α), and Early B-Cell Factor-two (EBF2).[72] [73] [74]
The listing of molecules that influence browning has grown in straight proportion to the popularity of this topic and is constantly evolving every bit more knowledge is acquired. Among these molecules are irisin and fibroblast growth factor 21 (FGF21), which accept been well-studied and are believed to exist important regulators of browning. Irisin is secreted from muscle in response to practise and has been shown to increase browning by interim on beige preadipocytes.[75] FGF21, a hormone secreted mainly past the liver, has garnered a not bad deal of interest subsequently being identified as a potent stimulator of glucose uptake and a browning regulator through its effects on PGC-1α.[66] Information technology is increased in BAT during common cold exposure and is thought to assist in resistance to diet-induced obesity[76] FGF21 may also be secreted in response to exercise and a low protein nutrition, although the latter has not been thoroughly investigated.[77] [78] Data from these studies propose that ecology factors similar diet and exercise may be important mediators of browning. In mice, it was found that beiging can occur through the production of methionine-enkephalin peptides past type 2 innate lymphoid cells in response to interleukin 33.[79]
Genomics and bioinformatics tools to report browning [edit]
Due to the complex nature of adipose tissue and a growing list of browning regulatory molecules, great potential exists for the utilise of bioinformatics tools to meliorate written report within this field. Studies of WAT browning have profoundly benefited from advances in these techniques, as beige fat is rapidly gaining popularity every bit a therapeutic target for the handling of obesity and diabetes.
DNA microarray is a bioinformatics tool used to quantify expression levels of various genes simultaneously, and has been used extensively in the study of adipose tissue. One such study used microarray analysis in conjunction with Ingenuity IPA software to await at changes in WAT and BAT gene expression when mice were exposed to temperatures of 28 and vi °C.[lxxx] The most significantly upwardly- and downregulated genes were and so identified and used for analysis of differentially expressed pathways. Information technology was discovered that many of the pathways upregulated in WAT after common cold exposure are also highly expressed in BAT, such equally oxidative phosphorylation, fatty acid metabolism, and pyruvate metabolism.[lxxx] This suggests that some of the adipocytes switched to a beige phenotype at 6 °C. Mössenböck et al. also used microarray analysis to demonstrate that insulin deficiency inhibits the differentiation of beige adipocytes but does not disturb their capacity for browning.[81] These ii studies demonstrate the potential for the use of microarray in the study of WAT browning.
RNA sequencing (RNA-Seq) is a powerful computational tool that allows for the quantification of RNA expression for all genes within a sample. Incorporating RNA-Seq into browning studies is of great value, as information technology offers better specificity, sensitivity, and a more comprehensive overview of cistron expression than other methods. RNA-Seq has been used in both human being and mouse studies in an attempt narrate beige adipocytes according to their gene expression profiles and to identify potential therapeutic molecules that may induce the beige phenotype. One such study used RNA-Seq to compare cistron expression profiles of WAT from wild-type (WT) mice and those overexpressing Early B-Cell Factor-2 (EBF2). WAT from the transgenic animals exhibited a brown fat factor plan and had decreased WAT specific gene expression compared to the WT mice.[82] Thus, EBF2 has been identified as a potential therapeutic molecule to induce beiging.
Chromatin immunoprecipitation with sequencing (ChIP-seq) is a method used to identify poly peptide binding sites on DNA and assess histone modifications. This tool has enabled exam of epigenetic regulation of browning and helps elucidate the mechanisms by which poly peptide-Dna interactions stimulate the differentiation of biscuit adipocytes. Studies observing the chromatin landscapes of beige adipocytes accept found that adipogenesis of these cells results from the germination of cell specific chromatin landscapes, which regulate the transcriptional plan and, ultimately, control differentiation. Using Flake-seq in conjunction with other tools, recent studies accept identified over thirty transcriptional and epigenetic factors that influence beige adipocyte development.[82]
Genetics [edit]
The thrifty cistron hypothesis (also called the dearth hypothesis) states that in some populations the trunk would be more efficient at retaining fat in times of plenty, thereby endowing greater resistance to starvation in times of food scarcity. This hypothesis, originally avant-garde in the context of glucose metabolism and insulin resistance, has been discredited by physical anthropologists, physiologists, and the original proponent of the idea himself with respect to that context, although according to its developer it remains "every bit feasible as when [information technology was] start avant-garde" in other contexts.[83] [84]
In 1995, Jeffrey Friedman, in his residency at the Rockefeller University, together with Rudolph Leibel, Douglas Coleman et al. discovered the protein leptin that the genetically obese mouse lacked.[85] [86] [87] Leptin is produced in the white adipose tissue and signals to the hypothalamus. When leptin levels drop, the torso interprets this as a loss of free energy, and hunger increases. Mice lacking this protein eat until they are four times their normal size.
Leptin, however, plays a different role in diet-induced obesity in rodents and humans. Because adipocytes produce leptin, leptin levels are elevated in the obese. However, hunger remains, and—when leptin levels drop due to weight loss—hunger increases. The drop of leptin is better viewed as a starvation signal than the rise of leptin as a satiety betoken.[88] Notwithstanding, elevated leptin in obesity is known as leptin resistance. The changes that occur in the hypothalamus to result in leptin resistance in obesity are currently the focus of obesity research.[89]
Cistron defects in the leptin gene (ob) are rare in human obesity.[xc] Equally of July 2010[update], just xiv individuals from five families accept been identified worldwide who bear a mutated ob cistron (one of which was the first e'er identified cause of genetic obesity in humans)—ii families of Pakistani origin living in the United kingdom of great britain and northern ireland, one family living in Turkey, one in Arab republic of egypt, and one in Republic of austria[91] [92] [93] [94] [95]—and 2 other families have been found that acquit a mutated ob receptor.[96] [97] Others have been identified as genetically partially deficient in leptin, and, in these individuals, leptin levels on the low finish of the normal range can predict obesity.[98]
Several mutations of genes involving the melanocortins (used in brain signaling associated with appetite) and their receptors have also been identified as causing obesity in a larger portion of the population than leptin mutations.[99]
Physical properties [edit]
Adipose tissue has a density of ~0.ix grand/ml.[100] Thus, a person with more than adipose tissue volition float more hands than a person of the same weight with more than muscular tissue, since muscular tissue has a density of 1.06 g/ml.[101]
Body fat meter [edit]
A trunk fat meter is a tool used to measure out the body fatty to weight ratio in the man trunk. Unlike meters use various methods to determine the ratio. They tend to under-read torso fat percentage.
In contrast with clinical tools, one relatively cheap type of torso fat meter uses the principle of bioelectrical impedance analysis (BIA) in order to determine an individual's torso fat percentage. To achieve this, the meter passes a small-scale, harmless, electric current through the torso and measures the resistance, and then uses information on the person's weight, height, age, and sex activity to calculate an approximate value for the person's body fatty percent. The calculation measures the full volume of h2o in the body (lean tissue and muscle contain a higher pct of water than fat), and estimates the percentage of fat based on this information. The result can fluctuate several percentage points depending on what has been eaten and how much water has been drunkard earlier the analysis.
Before bioelectrical impedance assay machines were developed, there were many dissimilar ways in analyzing body composition such equally skin fold methods using calipers, underwater weighing, whole body air displacement plethysmography (ADP) and DXA.
Brute studies [edit]
Within the fatty (adipose) tissue of CCR2 scarce mice, at that place is an increased number of eosinophils, greater alternative Macrophage activation, and a propensity towards type 2 cytokine expression. Furthermore, this effect was exaggerated when the mice became obese from a high fat diet.[102]
Gallery [edit]
-

Diagrammatic exclusive view of the skin (magnified).
-

White adipose tissue in paraffin department
-

Electronic musical instrument of body fatty meter
See too [edit]
- Adipose differentiation-related poly peptide
- Adipocytes
- Apelin
- Bioelectrical impedance analysis – a method to measure body fatty percentage.
- Blab – an extra thick form of adipose tissue found in some marine mammals.
- Trunk fatty pct
- Cellulite
- Lipolysis
- Lipodystrophy
- Human fat used every bit pharmaceutical in traditional medicine
- Obesity
- Starvation
- Steatosis (also chosen fatty modify, fatty degeneration or adipose degeneration)
- Stem cells
- Subcutaneous fatty
- Bariatrics
- Classification of obesity
- Classification of childhood obesity
- EPODE International Network, the world'due south largest obesity-prevention network
- World Fit A program of the United States Olympic Committee (USOC), and the U.s.a. Olympians and Paralympians Association (USOP)
- Obesity and walking
- Social stigma of obesity
References [edit]
- ^ a b c d Birbrair A, Zhang T, Wang ZM, Messi ML, Enikolopov GN, Mintz A, Delbono O (Baronial 2013). "Office of pericytes in skeletal muscle regeneration and fatty accumulation". Stem Cells and Development. 22 (16): 2298–314. doi:10.1089/scd.2012.0647. PMC3730538. PMID 23517218.
- ^ Kershaw EE, Flier JS (June 2004). "Adipose tissue as an endocrine organ". The Periodical of Clinical Endocrinology and Metabolism. 89 (vi): 2548–56. doi:10.1210/jc.2004-0395. PMID 15181022.
- ^ Mancuso P (May 2016). "The role of adipokines in chronic inflammation". ImmunoTargets and Therapy. 5 (2016): 47–56. doi:x.2147/ITT.S73223. PMID 27529061.
- ^ Cannon B, Nedergaard J (Baronial 2008). "Developmental biology: Neither fat nor mankind". Nature. 454 (7207): 947–48. Bibcode:2008Natur.454..947C. doi:10.1038/454947a. PMID 18719573. S2CID 205040511.
- ^ Aarsland A, Chinkes D, Wolfe RR (June 1997). "Hepatic and whole-torso fatty synthesis in humans during saccharide overfeeding". The American Journal of Clinical Nutrition. 65 (half-dozen): 1774–82. doi:10.1093/ajcn/65.6.1774. PMID 9174472.
- ^ Pond CM (1998). The Fats of Life . Cambridge University Press. ISBN978-0-521-63577-6.
- ^ Cinti S (July 2005). "The adipose organ". Prostaglandins, Leukotrienes, and Essential Fatty Acids. 73 (ane): 9–15. doi:10.1016/j.plefa.2005.04.010. PMID 15936182.
- ^ Bachmanov AA, Reed DR, Tordoff MG, Price RA, Beauchamp GK (March 2001). "Nutrient preference and nutrition-induced adiposity in C57BL/6ByJ and 129P3/J mice". Physiology & Behavior. 72 (4): 603–13. doi:10.1016/S0031-9384(01)00412-vii. PMC3341942. PMID 11282146.
- ^ Wirth, Alfred; Wabitsch, Martin; Hauner, Hans (October 2014). "The Prevention and Treatment of Obesity". Deutsches Ärzteblatt International. 111 (42): 705–713. doi:x.3238/arztebl.2014.0705. ISSN 1866-0452. PMC4233761. PMID 25385482.
- ^ Fat on the Inside: Looking Thin is Not Enough, By Fiona Haynes, About.com
- ^ a b "Abdominal fat and what to do nigh it". President & Fellows of Harvard College. September 2005.
Visceral fat more of a wellness concern than subcutaneous fat
- ^ Nagai M, Komiya H, Mori Y, Ohta T, Kasahara Y, Ikeda Y (May 2010). "Estimating visceral fat area past multifrequency bioelectrical impedance". Diabetes Care. 33 (5): 1077–79. doi:10.2337/dc09-1099. PMC2858179. PMID 20150289.
- ^ Montague CT, O'Rahilly S (June 2000). "The perils of portliness: causes and consequences of visceral adiposity". Diabetes. 49 (vi): 883–88. doi:10.2337/diabetes.49.6.883. PMID 10866038.
- ^ Kern PA, Ranganathan S, Li C, Wood L, Ranganathan G (May 2001). "Adipose tissue tumor necrosis factor and interleukin-6 expression in human obesity and insulin resistance". American Journal of Physiology. Endocrinology and Metabolism. 280 (5): E745–51. doi:ten.1152/ajpendo.2001.280.5.e745. PMID 11287357. S2CID 24306481.
- ^ Marette A (Dec 2003). "Molecular mechanisms of inflammation in obesity-linked insulin resistance". International Journal of Obesity and Related Metabolic Disorders. 27 Suppl iii: S46–48. doi:10.1038/sj.ijo.0802500. PMID 14704744.
- ^ Mokdad AH, Ford ES, Bowman BA, Dietz WH, Vinicor F, Bales VS, et al. (January 2003). "Prevalence of obesity, diabetes, and obesity-related wellness chance factors, 2001". JAMA. 289 (1): 76–79. doi:10.1001/jama.289.1.76. PMID 12503980.
- ^ Maresky HS, Sharfman Z, Ziv-Baran T, Gomori JM, Copel L, Tal Due south (Nov 2015). "Anthropometric Assessment of Neck Adipose Tissue and Airway Book Using Multidetector Computed Tomography: An Imaging Approach and Clan With Overall Bloodshed". Medicine. 94 (45): e1991. doi:10.1097/Doctor.0000000000001991. PMC4912280. PMID 26559286.
- ^ Chocolate-brown JC, Harhay MO, Harhay MN (2016). "Anthropometrically predicted visceral adipose tissue and blood-based biomarkers: a cross-exclusive assay". European Journal of Nutrition. 57 (1): 191–198. doi:10.1007/s00394-016-1308-viii. PMC5513780. PMID 27614626.
- ^ Chocolate-brown JC, Harhay MO, Harhay MN (2017). "Anthropometrically-predicted visceral adipose tissue and mortality amidst men and women in the third national health and nutrition examination survey (NHANES 3)". American Journal of Human Biology. 29 (1): e22898. doi:10.1002/ajhb.22898. PMC5241265. PMID 27427402.
- ^ "Reduce Abdominal Fatty". Archived from the original on 2011-09-28. Retrieved 2009-04-10 .
Estrogen causes fat to be stored around the pelvic region, hips, butt and thighs (pelvic region)
- ^ "Waistline Worries: Turning Apples Back Into Pears". healthywomen.org. Archived from the original on 2009-06-09.
- ^ Researchers think that the lack of estrogen at menopause plays a part in driving our fat n. See: Andrews, Michelle (2006-12-01). "A Matter of Fat". Yahoo Health. Women's Health. Archived from the original on 2007-03-15.
- ^ Singh, Ajay Thousand.; Loscalzo, Joseph, eds. (2014). The Brigham Intensive Review of Internal Medicine (2d ed.). New York, NY: Oxford Academy Press. p. 483. ISBN978-0-19-935827-4 . Retrieved August 3, 2021.
- ^ Ohkawara K, Tanaka Due south, Miyachi M, Ishikawa-Takata K, Tabata I (December 2007). "A dose-response relation between aerobic exercise and visceral fatty reduction: systematic review of clinical trials". International Periodical of Obesity. 31 (12): 1786–97. doi:10.1038/sj.ijo.0803683. PMID 17637702.
- ^ Khalafi, Mousa; Malandish, Abbas; Rosenkranz, Sara One thousand.; Ravasi, Ali A. (May 16, 2021). "Effect of resistance training with and without caloric restriction on visceral fatty: A systemic review and meta-analysis". Obesity Reviews. 22 (9): e13275. doi:10.1111/obr.13275. PMID 33998135. S2CID 234747534. Retrieved Baronial iii, 2021.
- ^ Verheggen, R. J. H. Grand.; Maessen, Yard. F. H.; Green, D. J.; Hermus, A. R. M. M.; Hopman, K. T. E.; Thijssen, D. H. T. (Baronial 2016). "A systematic review and meta-analysis on the effects of exercise training versus hypocaloric diet: distinct effects on body weight and visceral adipose tissue". Obesity Reviews. 17 (8): 664–690. doi:ten.1111/obr.12406. PMID 27213481. S2CID 206228752. Retrieved August 3, 2021.
- ^ Irving BA, Davis CK, Brock DW, Weltman JY, Swift D, Barrett EJ, Gaesser GA, Weltman A (November 2008). "Event of exercise training intensity on abdominal visceral fatty and torso composition". Medicine and Science in Sports and Exercise. 40 (eleven): 1863–72. doi:10.1249/MSS.0b013e3181801d40. PMC2730190. PMID 18845966.
- ^ Coker RH, Williams RH, Kortebein PM, Sullivan DH, Evans WJ (Baronial 2009). "Influence of exercise intensity on abdominal fat and adiponectin in elderly adults". Metabolic Syndrome and Related Disorders. 7 (4): 363–68. doi:10.1089/met.2008.0060. PMC3135883. PMID 19196080.
- ^ R, Ross; J, Rissanen (Nov 1994). "Mobilization of Visceral and Subcutaneous Adipose Tissue in Response to Free energy Restriction and Do". The American Periodical of Clinical Nutrition. 60 (v): 695–703. doi:10.1093/ajcn/60.5.695. PMID 7942575. Retrieved 2020-06-05 .
- ^ Mazurek T, Zhang L, Zalewski A, Mannion JD, Diehl JT, Arafat H, Sarov-Blat L, O'Brien Due south, Keiper EA, Johnson AG, Martin J, Goldstein BJ, Shi Y, et al. (November 2003). "Human epicardial adipose tissue is a source of inflammatory mediators". Circulation. 108 (20): 2460–66. doi:10.1161/01.CIR.0000099542.57313.C5. PMID 14581396.
- ^ Pezeshkian M, Noori 1000, Najjarpour-Jabbari H, Abolfathi A, Darabi 1000, Darabi Yard, Shaaker K, Shahmohammadi 1000, et al. (Apr 2009). "Fatty acid composition of epicardial and subcutaneous man adipose tissue". Metabolic Syndrome and Related Disorders. 7 (2): 125–31. doi:ten.1089/met.2008.0056. PMID 19422139.
- ^ a b Hoehn Yard, Marieb EN (2008). Beefcake & Physiology (3rd ed.). San Francisco, Calif.: Pearson/Benjamin Cummings. ISBN978-0-8053-0094-nine.
- ^ Porter SA, Massaro JM, Hoffmann U, Vasan RS, O'Donnel CJ, Fox CS (June 2009). "Abdominal subcutaneous adipose tissue: a protective fat depot?". Diabetes Care. 32 (6): 1068–75. doi:10.2337/dc08-2280. PMC2681034. PMID 19244087.
- ^ "Abdomen fat in women: Taking – and keeping – it off". MayoClinic.com. 2013-06-08. Retrieved 2013-12-02 .
- ^ Frayn, Chiliad. N.; Karpe, F.; Manolopoulos, K. N. (June 2010). "Gluteofemoral body fat as a determinant of metabolic wellness". International Periodical of Obesity. 34 (6): 949–959. doi:ten.1038/ijo.2009.286. ISSN 1476-5497. PMID 20065965.
- ^ a b Brodie D, Moscrip V, Hutcheon R (March 1998). "Torso composition measurement: a review of hydrodensitometry, anthropometry, and impedance methods". Nutrition. fourteen (three): 296–310. doi:10.1016/S0899-9007(97)00474-seven. PMID 9583375.
- ^ Devlin MJ, Cloutier AM, Thomas NA, Panus DA, Lotinun S, Pinz I, Businesswoman R, Rosen CJ, Bouxsein ML (September 2010). "Caloric restriction leads to high marrow adiposity and low bone mass in growing mice". Journal of Bone and Mineral Research. 25 (9): 2078–88. doi:x.1002/jbmr.82. PMC3127399. PMID 20229598.
- ^ Cawthorn WP, Scheller EL, Parlee SD, Pham HA, Learman BS, Redshaw CM, Sulston RJ, Burr AA, Das AK, Simon BR, Mori H, Bree AJ, Schell B, Krishnan V, MacDougald OA (February 2016). "Expansion of Os Marrow Adipose Tissue During Caloric Restriction Is Associated With Increased Circulating Glucocorticoids and Not With Hypoleptinemia". Endocrinology. 157 (two): 508–21. doi:ten.1210/en.2015-1477. PMC4733126. PMID 26696121.
- ^ Bredella MA, Fazeli PK, Miller KK, Misra M, Torriani K, Thomas BJ, Ghomi RH, Rosen CJ, Klibanski A (June 2009). "Increased bone marrow fat in anorexia nervosa". The Journal of Clinical Endocrinology and Metabolism. 94 (6): 2129–36. doi:ten.1210/jc.2008-2532. PMC2690416. PMID 19318450.
- ^ a b Styner One thousand, Pagnotti GM, McGrath C, Wu 10, Sen B, Uzer 1000, Xie Z, Zong X, Styner MA, Rubin CT, Rubin J (August 2017). "Exercise Decreases Marrow Adipose Tissue through β-Oxidation in Obese Running Mice". Periodical of Os and Mineral Research. 32 (8): 1692–702. doi:ten.1002/jbmr.3159. PMC5550355. PMID 28436105.
- ^ Styner 1000, Pagnotti GM, Galior K, Wu X, Thompson WR, Uzer Chiliad, Sen B, Xie Z, Horowitz MC, Styner MA, Rubin C, Rubin J (August 2015). "Practise Regulation of Marrow Fatty in the Setting of PPARγ Agonist Treatment in Female C57BL/6 Mice". Endocrinology. 156 (eight): 2753–61. doi:10.1210/en.2015-1213. PMC4511140. PMID 26052898.
- ^ Styner M, Thompson WR, Galior G, Uzer G, Wu X, Kadari S, Case North, Xie Z, Sen B, Romaine A, Pagnotti GM, Rubin CT, Styner MA, Horowitz MC, Rubin J (July 2014). "Bone marrow fat accumulation accelerated by loftier fat nutrition is suppressed by exercise". Bone. 64: 39–46. doi:10.1016/j.bone.2014.03.044. PMC4041820. PMID 24709686.
- ^ a b Snel G, Jonker JT, Schoones J, Lamb H, de Roos A, Pijl H, Smit JW, Meinders AE, Jazet IM (2012). "Ectopic fat and insulin resistance: pathophysiology and effect of diet and lifestyle interventions". International Periodical of Endocrinology. 2012: one–eighteen. doi:x.1155/2012/983814. PMC3366269. PMID 22675355.
- ^ Hens W, Vissers D, Hansen D, Peeters S, Gielen J, Van Gaal L, Taeymans J (2017). "The effect of diet or practice on ectopic adiposity in children and adolescents with obesity: a systematic review and meta-assay". Obesity Reviews. 18 (eleven): 1310–22. doi:10.1111/obr.12577. hdl:1942/24948. PMID 28913977. S2CID 10876113.
- ^ Hens W, Taeyman J, Cornelis J, Gielen J, Van Gaal L, Vissers D (2016). "The Effect of Lifestyle Interventions on Excess Ectopic Fat Degradation Measured by Noninvasive Techniques in Overweight and Obese Adults: A Systematic Review and Meta-Analysis". Periodical of Physical Action and Wellness. 13 (6): 671–94. doi:10.1123/jpah.2015-0560. hdl:10067/1321600151162165141. PMID 26694194.
- ^ Thomas, Lorette W. (1962-04-07). "The Chemical Composition of Adipose Tissue of Man and Mice". Quarterly Journal of Experimental Physiology and Cognate Medical Sciences. 47 (2): 179–188. doi:10.1113/expphysiol.1962.sp001589. ISSN 1469-445X. PMID 13920823.
- ^ Amitani, Marie; Asakawa, Akihiro; Amitani, Haruka; Inui, Akio (2013). "The role of leptin in the command of insulin-glucose centrality". Frontiers in Neuroscience. seven: 51. doi:ten.3389/fnins.2013.00051. ISSN 1662-453X. PMC3619125. PMID 23579596.
- ^ Dhaliwal SS, Welborn TA (2009). "Central obesity and multivariable cardiovascular risk as assessed by the Framingham prediction scores". Am J Cardiol. 103 (10): 1403–07. doi:10.1016/j.amjcard.2008.12.048. PMID 19427436.
- ^ Park A (2009-08-08). "Fatty-Bellied Monkeys Suggest Why Stress Sucks". Time. Archived from the original on December 20, 2013. Retrieved 2013-12-19 .
- ^ Sugii S, Kida Y, Kawamura T, Suzuki J, Vassena R, Yin YQ, et al. (February 2010). "Homo and mouse adipose-derived cells support feeder-independent induction of pluripotent stalk cells". Proceedings of the National University of Sciences. 107 (8): 3558–63. Bibcode:2010PNAS..107.3558S. doi:ten.1073/pnas.0910172106. PMC2840462. PMID 20133714.
- ^ a b Atzmon G, Yang XM, Muzumdar R, Ma XH, Gabriely I, Barzilai Northward (November 2002). "Differential factor expression between visceral and subcutaneous fatty depots". Hormone and Metabolic Research. 34 (11–12): 622–28. doi:10.1055/s-2002-38250. PMID 12660871.
- ^ Baglioni S, Cantini G, Poli Chiliad, Francalanci M, Squecco R, Di Franco A, Borgogni E, Frontera South, Nesi One thousand, Liotta F, Lucchese Thou, Perigli 1000, Francini F, Forti G, Serio M, Luconi Thousand (4 May 2012). "Functional differences in visceral and subcutaneous fat pads originate from differences in the adipose stem cell". PLOS One. 7 (5): e36569. Bibcode:2012PLoSO...736569B. doi:ten.1371/journal.pone.0036569. PMC3344924. PMID 22574183.
- ^ Russo V, Yu C, Belliveau P, Hamilton A, Flynn LE (February 2014). "Comparison of human adipose-derived stalk cells isolated from subcutaneous, omental, and intrathoracic adipose tissue depots for regenerative applications". Stem Cells Translational Medicine. 3 (2): 206–17. doi:x.5966/sctm.2013-0125. PMC3925056. PMID 24361924.
- ^ Lempesis, Ioannis K.; Meijel, Rens 50. J. van; Manolopoulos, Konstantinos N.; Goossens, Gijs H. (2019). "Oxygenation of adipose tissue: A man perspective". Acta Physiologica. 228 (one): e13298. doi:10.1111/apha.13298. ISSN 1748-1716. PMC6916558. PMID 31077538.
- ^ Stocco, Carlos (Jan 2012). "Tissue Physiology and Pathology of Aromatase". Steroids. 77 (1–2): 27–35. doi:10.1016/j.steroids.2011.10.013. ISSN 0039-128X. PMC3286233. PMID 22108547.
- ^ Löhn M, Dubrovska M, Lauterbach B, Luft FC, Gollasch K, Sharma AM (July 2002). "Periadventitial fat releases a vascular relaxing factor". FASEB Periodical. 16 (9): 1057–63. doi:10.1096/fj.02-0024com. PMID 12087067. S2CID 902537.
- ^ a b Cannon B, Nedergaard J (Jan 2004). "Brown adipose tissue: role and physiological significance". Physiological Reviews. 84 (one): 277–359. doi:x.1152/physrev.00015.2003. PMID 14715917. S2CID 14289041.
- ^ Busiello RA, Savarese Due south, Lombardi A (2015). "Mitochondrial uncoupling proteins and energy metabolism". Frontiers in Physiology. 6 (36): 36. doi:10.3389/fphys.2015.00036. PMC4322621. PMID 25713540.
- ^ Fedorenko A, Lishko PV, Kirichok Y (Oct 2012). "Mechanism of fat-acrid-dependent UCP1 uncoupling in brown fat mitochondria". Cell. 151 (2): 400–thirteen. doi:10.1016/j.cell.2012.09.010. PMC3782081. PMID 23063128.
- ^ Azzu V, Brand Doctor (May 2010). "The on-off switches of the mitochondrial uncoupling proteins". Trends in Biochemical Sciences. 35 (5): 298–307. doi:10.1016/j.tibs.2009.11.001. PMC3640847. PMID 20006514.
- ^ Samuelson, Isabella; Vidal-Puig, Antonio (2020). "Studying Dark-brown Adipose Tissue in a Human being in vitro Context". Frontiers in Endocrinology. 11: 629. doi:10.3389/fendo.2020.00629. ISSN 1664-2392. PMC7523498. PMID 33042008.
- ^ Nedergaard J, Bengtsson T, Cannon B (August 2007). "Unexpected evidence for active brown adipose tissue in adult humans". American Periodical of Physiology. Endocrinology and Metabolism. 293 (2): E444–52. doi:x.1152/ajpendo.00691.2006. PMID 17473055. S2CID 230947.
- ^ Virtanen KA, Lidell ME, Orava J, Heglind G, Westergren R, Niemi T, et al. (Apr 2009). "Functional brown adipose tissue in good for you adults". The New England Periodical of Medicine. 360 (15): 1518–25. doi:ten.1056/NEJMoa0808949. PMID 19357407.
- ^ van Marken Lichtenbelt WD, Vanhommerig JW, Smulders NM, Drossaerts JM, Kemerink GJ, Bouvy ND, et al. (April 2009). "Cold-activated brown adipose tissue in healthy men". The New England Journal of Medicine. 360 (fifteen): 1500–08. doi:10.1056/NEJMoa0808718. PMID 19357405. S2CID 477352.
- ^ Cypess AM, Lehman S, Williams Thousand, Tal I, Rodman D, Goldfine AB, et al. (Apr 2009). "Identification and importance of brown adipose tissue in adult humans". The New England Journal of Medicine. 360 (15): 1509–17. doi:10.1056/NEJMoa0810780. PMC2859951. PMID 19357406.
- ^ a b c Harms M, Seale P (October 2013). "Brownish and beige fatty: development, office and therapeutic potential". Nature Medicine. nineteen (10): 1252–63. doi:x.1038/nm.3361. PMID 24100998.
- ^ Cypess AM, Kahn CR (Apr 2010). "Brownish fatty as a therapy for obesity and diabetes". Current Opinion in Endocrinology, Diabetes and Obesity. 17 (two): 143–49. doi:10.1097/MED.0b013e328337a81f. PMC3593105. PMID 20160646.
- ^ Gospodarska Eastward, Nowialis P, Kozak LP (March 2015). "Mitochondrial turnover: a phenotype distinguishing brown adipocytes from interscapular chocolate-brown adipose tissue and white adipose tissue". The Journal of Biological Chemical science. 290 (13): 8243–55. doi:ten.1074/jbc.M115.637785. PMC4375480. PMID 25645913.
- ^ Rosenwald K, Perdikari A, Rülicke T, Wolfrum C (June 2013). "Bi-directional interconversion of brite and white adipocytes". Nature Cell Biology. fifteen (half dozen): 659–67. doi:10.1038/ncb2740. PMID 23624403. S2CID 2842953.
- ^ Lo KA, Sun 50 (September 2013). "Turning WAT into BAT: a review on regulators controlling the browning of white adipocytes". Bioscience Reports. 33 (5): 711–19. doi:10.1042/BSR20130046. PMC3764508. PMID 23895241.
- ^ Harms MJ, Ishibashi J, Wang W, Lim HW, Goyama South, Sato T, Kurokawa M, Won KJ, Seale P (April 2014). "Prdm16 is required for the maintenance of dark-brown adipocyte identity and office in adult mice". Cell Metabolism. xix (four): 593–604. doi:x.1016/j.cmet.2014.03.007. PMC4012340. PMID 24703692.
- ^ Wang Westward, Kissig One thousand, Rajakumari Due south, Huang L, Lim HW, Won KJ, Seale P (October 2014). "Ebf2 is a selective marker of chocolate-brown and beige adipogenic precursor cells". Proceedings of the National Academy of Sciences. 111 (forty): 14466–71. Bibcode:2014PNAS..11114466W. doi:10.1073/pnas.1412685111. PMC4209986. PMID 25197048.
- ^ Kissig M, Shapira SN, Seale P (June 2016). "SnapShot: Brown and Beige Adipose Thermogenesis". Prison cell. 166 (one): 258–258.e1. doi:x.1016/j.jail cell.2016.06.038. PMC5478388. PMID 27368105.
- ^ Shapira SN, Lim HW, Rajakumari S, Sakers AP, Ishibashi J, Harms MJ, Won KJ, Seale P (April 2017). "EBF2 transcriptionally regulates dark-brown adipogenesis via the histone reader DPF3 and the BAF chromatin remodeling circuitous". Genes & Development. 31 (7): 660–73. doi:10.1101/gad.294405.116. PMC5411707. PMID 28428261.
- ^ Boström P, Wu J, Jedrychowski MP, Korde A, Ye Fifty, Lo JC, Rasbach KA, Boström EA, Choi JH, Long JZ, Kajimura S, Zingaretti MC, Vind BF, Tu H, Cinti S, Højlund K, Gygi SP, Spiegelman BM (January 2012). "A PGC1-α-dependent myokine that drives brown-fat-like development of white fatty and thermogenesis". Nature. 481 (7382): 463–68. Bibcode:2012Natur.481..463B. doi:10.1038/nature10777. PMC3522098. PMID 22237023.
- ^ Ohta H, Itoh N (2014). "Roles of FGFs as Adipokines in Adipose Tissue Development, Remodeling, and Metabolism". Frontiers in Endocrinology. 5 (18): xviii. doi:10.3389/fendo.2014.00018. PMC3932445. PMID 24605108.
- ^ Fenzl A, Kiefer FW (July 2014). "Chocolate-brown adipose tissue and thermogenesis". Hormone Molecular Biology and Clinical Investigation. xix (1): 25–37. doi:10.1515/hmbci-2014-0022. PMID 25390014. S2CID 35008082.
- ^ Laeger T, Henagan TM, Albarado DC, Redman LM, Bray GA, Noland RC, Münzberg H, Hutson SM, Gettys TW, Schwartz MW, Morrison CD (September 2014). "FGF21 is an endocrine bespeak of protein restriction". The Journal of Clinical Investigation. 124 (ix): 3913–22. doi:ten.1172/JCI74915. PMC4153701. PMID 25133427.
- ^ Brestoff, Jonathan R.; Kim, Brian Southward.; Saenz, Steven A.; Stine, Rachel R.; Monticelli, Laurel A.; Sonnenberg, Gregory F.; Thome, Joseph J.; Farber, Donna L.; Lutfy, Kabirullah (12 March 2015). "Group two innate lymphoid cells promote beiging of white adipose tissue and limit obesity". Nature. 519 (7542): 242–246. Bibcode:2015Natur.519..242B. doi:x.1038/nature14115. ISSN 1476-4687. PMC4447235. PMID 25533952.
- ^ a b Rosell Thou, Kaforou Yard, Frontini A, Okolo A, Chan YW, Nikolopoulou E, Millership Southward, Fenech ME, MacIntyre D, Turner JO, Moore JD, Blackburn East, Gullick WJ, Cinti South, Montana G, Parker MG, Christian M (Apr 2014). "Brown and white adipose tissues: intrinsic differences in factor expression and response to cold exposure in mice". American Journal of Physiology. Endocrinology and Metabolism. 306 (8): E945–64. doi:ten.1152/ajpendo.00473.2013. PMC3989735. PMID 24549398.
- ^ Inagaki T, Sakai J, Kajimura S (August 2016). "Transcriptional and epigenetic control of brown and beige adipose cell fate and function". Nature Reviews Molecular Cell Biological science. 17 (viii): 480–95. doi:ten.1038/nrm.2016.62. PMC4956538. PMID 27251423.
- ^ a b Stine RR, Shapira SN, Lim HW, Ishibashi J, Harms M, Won KJ, Seale P (January 2016). "EBF2 promotes the recruitment of beige adipocytes in white adipose tissue". Molecular Metabolism. 5 (1): 57–65. doi:10.1016/j.molmet.2015.11.001. PMC4703852. PMID 26844207.
- ^ Speakerman JR (2007). "Genetics of Obesity: Five Fundamental Problems with the Famine Hypothesis". In Fantuzzi Grand, Mazzone T (eds.). Adipose Tissue and Adipokines in Wellness and Disease. Nutrition and Health. Humana Press. pp. 221–236. doi:10.1007/978-i-59745-370-7_17. ISBN978-1-58829-721-one.
- ^ Neel JV (1989). "The study of natural pick in archaic and civilized man populations. 1958". Human being Biological science. 61 (5–6): 781–810, discussion 811–23. PMID 2699601.
- ^ Vanquish East (Jan ane, 2002). "Chapter 4: On the Cutting Edge". The Hungry Gene: The Inside Story of the Obesity Manufacture. Atlantic Monthly Press. ISBN978-1-4223-5243-4.
- ^ Vanquish E (Jan i, 2002). "Affiliate v: Hunger". The Hungry Cistron: The Within Story of the Obesity Manufacture. Atlantic Monthly Press. ISBN978-1-4223-5243-4.
- ^ Pelleymounter MA, Cullen MJ, Baker MB, Hecht R, Winters D, Boone T, et al. (July 1995). "Effects of the obese gene production on body weight regulation in ob/ob mice". Scientific discipline. 269 (5223): 540–43. Bibcode:1995Sci...269..540P. doi:x.1126/science.7624776. PMID 7624776.
- ^ Ravussin E, Smith SR (2013). "Chapter xi: Role of the Adipocyte in Metabolism and Endocrine Function". In Weir GC, Jameson JL, De Groot LJ (eds.). Endocrinology Adult and Pediatric. Vol. Diabetes Mellitus and Obesity (6th ed.). Elsevier Wellness Sciences. ISBN978-0-323-22154-2. [ folio needed ]
- ^ Morris DL, Rui Fifty (Dec 2009). "Contempo advances in understanding leptin signaling and leptin resistance". American Journal of Physiology. Endocrinology and Metabolism. 297 (6): E1247–59. doi:10.1152/ajpendo.00274.2009. PMC2793049. PMID 19724019.
- ^ Carlsson B, Lindell K, Gabrielsson B, Karlsson C, Bjarnason R, Westphal O, et al. (January 1997). "Obese (ob) gene defects are rare in human obesity". Obesity Inquiry. 5 (ane): 30–35. doi:10.1002/j.1550-8528.1997.tb00280.x. PMID 9061713.
- ^ Montague CT, Farooqi IS, Whitehead JP, Soos MA, Rau H, Wareham NJ, Sewter CP, Digby JE, Mohammed SN, Hurst JA, Cheetham CH, Earley AR, Barnett AH, Prins JB, O'Rahilly S (June 1997). "Built leptin deficiency is associated with severe early-onset obesity in humans". Nature. 387 (6636): 903–eight. Bibcode:1997Natur.387..903M. doi:ten.1038/43185. PMID 9202122. S2CID 205032762.
- ^ Strobel A, Issad T, Camoin 50, Ozata M, Strosberg Advertisement (March 1998). "A leptin missense mutation associated with hypogonadism and morbid obesity". Nature Genetics. 18 (3): 213–fifteen. doi:x.1038/ng0398-213. PMID 9500540. S2CID 36920931.
- ^ Gibson WT, Farooqi IS, Moreau Chiliad, DePaoli AM, Lawrence Due east, O'Rahilly S, Trussell RA (October 2004). "Congenital leptin deficiency due to homozygosity for the Delta133G mutation: report of some other example and evaluation of response to iv years of leptin therapy". The Journal of Clinical Endocrinology and Metabolism. 89 (ten): 4821–26. doi:10.1210/jc.2004-0376. PMID 15472169.
- ^ Mazen I, El-Gammal M, Abdel-Hamid M, Amr K (August 2009). "A novel homozygous missense mutation of the leptin gene (N103K) in an obese Egyptian patient". Molecular Genetics and Metabolism. 97 (4): 305–08. doi:x.1016/j.ymgme.2009.04.002. PMID 19427251.
- ^ Fischer-Posovszky P, von Schnurbein J, Moepps B, Lahr Grand, Strauss One thousand, Barth TF, Kassubek J, Mühleder H, Möller P, Debatin KM, Gierschik P, Wabitsch 1000 (June 2010). "A new missense mutation in the leptin gene causes balmy obesity and hypogonadism without affecting T cell responsiveness". The Journal of Clinical Endocrinology and Metabolism. 95 (6): 2836–forty. doi:10.1210/jc.2009-2466. PMID 20382689.
- ^ Clément K, Vaisse C, Lahlou N, Cabrol Southward, Pelloux V, Cassuto D, Gourmelen K, Dina C, Chambaz J, Lacorte JM, Basdevant A, Bougnères P, Lebouc Y, Froguel P, Guy-G B (1998). "A mutation in the human leptin receptor gene causes obesity and pituitary dysfunction". Nature. 392 (6674): 398–401. Bibcode:1998Natur.392..398C. doi:10.1038/32911. PMID 9537324. S2CID 4400661.
- ^ Pankov YA (1999). "Adipose tissue as an endocrine organ regulating growth, puberty, and other physiological functions". Biochemistry. Biokhimiia. 64 (6): 601–09. PMID 10395972.
- ^ Farooqi IS, Keogh JM, Kamath Southward, Jones S, Gibson WT, Trussell R, Jebb SA, Lip GY, O'Rahilly Due south (November 2001). "Partial leptin deficiency and human adiposity". Nature. 414 (6859): 34–35. Bibcode:2001Natur.414...34F. doi:x.1038/35102112. PMID 11689931. S2CID 4344492.
- ^ Farooqi IS, O'Rahilly Southward (October 2008). "Mutations in ligands and receptors of the leptin-melanocortin pathway that lead to obesity". Nature Clinical Practice Endocrinology & Metabolism. 4 (10): 569–77. doi:ten.1038/ncpendmet0966. PMID 18779842. S2CID 13946212.
- ^ Farvid MS, Ng TW, Chan DC, Barrett PH, Watts GF (July 2005). "Clan of adiponectin and resistin with adipose tissue compartments, insulin resistance and dyslipidaemia". Diabetes, Obesity & Metabolism. 7 (4): 406–13. doi:10.1111/j.1463-1326.2004.00410.x. PMID 15955127. S2CID 46736884. (registration required)
- ^ Urbanchek MG, Picken EB, Kalliainen LK, Kuzon WM (May 2001). "Specific force deficit in skeletal muscles of former rats is partially explained by the being of denervated musculus fibers". The Journals of Gerontology. Series A, Biological Sciences and Medical Sciences. 56 (5): B191–97. doi:x.1093/gerona/56.5.B191. PMID 11320099.
- ^ Bolus WR, Gutierrez DA, Kennedy AJ, Anderson-Baucum EK, Hasty AH (Oct 2015). "CCR2 deficiency leads to increased eosinophils, alternative macrophage activation, and type 2 cytokine expression in adipose tissue". Journal of Leukocyte Biological science. 98 (4): 467–77. doi:x.1189/jlb.3HI0115-018R. PMC4763864. PMID 25934927. Archived from the original on 2017-05-09. Retrieved 2016-09-08 .
Further reading [edit]
- MeSH A10.165.114
- Stock MJ, Cinti S (2003). "Adipose Tissue / Structure and Function of Brown Adipose Tissue". Encyclopedia of Food Sciences and Nutrition. pp. 29–34. doi:x.1016/B0-12-227055-X/00008-0. ISBN978-0-12-227055-0.
- Vernon RG, Flint DJ (2003). "Adipose Tissue / Structure and Function of White Adipose Tissue". Encyclopedia of Food Sciences and Nutrition. pp. 23–29. doi:10.1016/B0-12-227055-X/00007-nine. ISBN978-0-12-227055-0.
External links [edit]
- Adipose tissue photomicrographs
Source: https://en.wikipedia.org/wiki/Adipose_tissue
Posted by: rivashoon1958.blogspot.com


0 Response to "Does Scar Tissue Register As Body Fat When Measured"
Post a Comment